A Three-Step Guide to Collecting More Patient Payments Up-Front
July 28, 2015 •Brian Watson

 Patient payment is evolving rapidly.
Patient payment is evolving rapidly.
From the rise in direct, out-of-pocket revenue to the transition to bundled care and value-based reimbursement models, healthcare providers are facing massive, transformational change in the way they collect and manage revenue.
A big part of that shift can be traced back to increased patient involvement with the financial side of care.
Over the last few years, deductibles have risen sharply for insured Americans, as more and more businesses embrace cost-sharing measures. Among all covered workers with a general annual deductible, the average deductible amount increased by 32% between 2009 and 2014.
And with employers eager to rein in health costs and avoid looming ‘Cadillac’ taxes on expensive plans, the popularity of Consumer-Directed Health Plans (CDHPs) is also booming. According to a 2014 Mercer study, last year saw the largest one-year increase in CDHP enrollment – from 18% to 23% of all covered employees. From the provider side, over 90% claim that high-deductible plans are becoming much more common in their hospitals and medical practices,
Looking ahead, almost a third of large employers plan to increase cost-sharing measures by making a CDHP their only benefit plan option this year – a year-over-year increase of nearly 50%.
Growth in public insurance marketplaces is also fueling the rising patient deductible creep. Of the 16.4 million patients enrolled through state and federal exchanges in 2014, almost 90% chose a high-deductible plan option.
All told, it’s projected that national patient out-of-pocket expenses will grow to more than $400 billion by 2016.
How Consumerism Is Changing Healthcare Payment
As patients transition from passive to active health consumers, their financial needs and expectations are changing. That development has several important implications for the future of patient payment.
One, more patients are now exposed to the financial implications of treatment. That means they’re looking to providers for help anticipating and managing the cost of care. As a result, transparent pricing and convenient financing options are becoming increasingly key patient financial tools.
Two, the number of patients with a balance-after-insurance is increasing.
On the surface at least, that second point has serious downside potential for providers. It takes more time and resources to collect from patients with an outstanding liability than payers. And follow-up is much more likely to have an adverse affect on consumer satisfaction and brand perception. Or fail altogether: nearly 50% of patient responsibility is never recovered.
But the rise in patient liability also offers a unique opportunity to permanently change how consumers think about paying for healthcare.
A patient payment model that moves financial activities to the front-end of treatment – during patient access and discharge – not only smoothes the transition from a deferred model to a faster, more efficient retail approach, it can also improve patient satisfaction by giving consumers the tools to better budget for, manage, and finance medical costs.
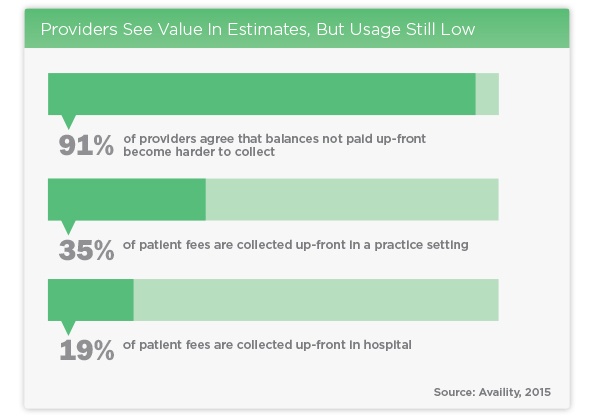
For those reasons, providers are overwhelmingly on board. Ninety-one percent of providers agree that patient payments not collected up-front become much harder to collect. Despite that enthusiasm, only 35% of patient fees are collected at the time of service in a physician practice setting. A similar situation exists in hospital collections, where just 19% of payments are collected up-front.
How do you increase point-of-service collections with already tight budgets? Let’s talk about a three-step process that can help you enhance and accelerate patient payment right now.
Anticipate
Transparency is critical for providers seeking to improve up-front collections.
Given the complex way healthcare is priced, it can be hard for consumers to accurately estimate the price of a doctor visit, outpatient procedure, or hospital stay – which makes anticipating and budgeting for medical bills tricky.
If patients don’t have a solid understanding of out-of-pocket costs before they’re asked for payment, your chances of collecting at the point of service are greatly reduced.
Sticker shock is common – especially for inexperienced healthcare consumers. And many patients simply lack the financial resources to pay a moderate-to-large balance due on the spot.
According to a recent Kaiser Family Foundation report, only 3 in 5 households have enough liquid assets to cover a $1,200 individual or $2,400 family deductible. In addition, consumers’ ability to pay for healthcare costs declined by over 11% during 2014.
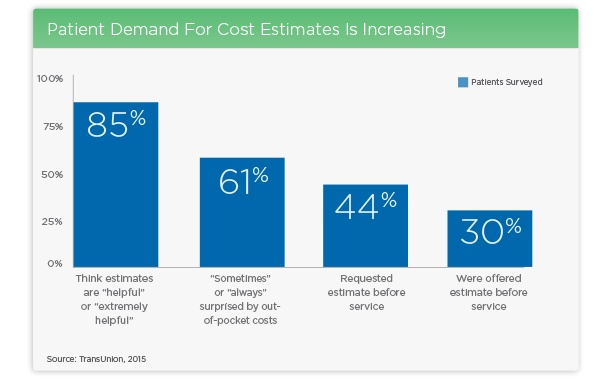
But despite complex underlying financial issues, a majority of patients are willing to pay when provided an accurate, good-faith estimate of treatment costs at or before the time of service. Research suggests that 57% of consumers would be willing to use a credit or debit card to cover out of pocket costs for a physicians’ visit of out-patient procedure if timely, actionable financial outreach was offered up-front.
Key Tools:
• Up-Front Estimates
Be proactive about educating patients on out-of-pocket costs prior to service. Not only do price estimates give patients the ability to compare providers and treatment options – and better manage the financial side of care – but they can also improve patient satisfaction and differentiate your hospital or practice from competitors.
• Responsive Communication
Engage patients prior to scheduled visits and outpatient procedures to initiate financial discussions. Estimates are only truly valuable if they can be used by patients to compare health options or plan for payment in advance of service. Follow-up on patient access with customized financial estimates via the consumer’s preferred channel – phone, text message, email, or mail.
Manage
Transparency in pre-service financial communication helps patients set expectations and control healthcare costs. But it can also improve how providers segment and connect with patients.
By combing a patient estimate with propensity to pay data, your financial staff can develop a fair, personalized payment roadmap for patients. For example, if a patient receives an estimate with a high balance due, but has a low propensity-to-pay score, they’re likely an ideal candidate for a specialized payment plan or financial counseling.
Blending payment estimates with financial analytics in this way helps providers improve financial outreach (and satisfaction) while ensuring that patients at risk for non-payment receive hands-on attention.
Key Tools:
• Propensity-to-Pay Analytics
Identify patients that would benefit from additional financial outreach before they leave your facility with propensity-to-pay analytics. This approach helps patients receive the structured financing they need – reducing bad debt and the risk to your brand from aggressive collections activities.
• Financial Outreach
Use effective, empathetic financial counseling in front-office areas or departments where self-pay balances after insurance are common – like emergency room.
Payment
According to a recent study from McKinsey and Company, if patients with insurance were given access to financing options and simpler ways to make a payment, only 10% of balance after insurance bad debt would remain uncollectable.
Fast, simple payment options support the move to more retail-like operations. By blending up-front pay tools with pre-service estimates and financial outreach, providers can increase cash collections, reduce A/R days, and lower costs.
Key Tools:
• Financing Programs
Special financing options – like interest-free payment plans – provide a fair, efficient way for self-pay patients to manage a balance that they might otherwise struggle to pay all at once. Interest-free options are especially patient-friendly, offering affordable terms – without the hidden fees and high interest rates of installment loans or credit cards.
• Clear Policy
It’s important that you set clear financial expectations for patients prior to service. Springing an unbudgeted expense can cause financial strain and even affect patient satisfaction with the treatment process. For example, almost three-quarters of patients who rated their care highly also had high praise for billing practices, while the nearly 70% that criticized their care also rated billing poorly.
Create a clear, written policy that lets patients know you will be asking for a portion of payment at the time of visit – and the consequences of non-payment. Then post the policy on your website and in registration areas. And communicate it during patient access and all pre-service financial outreach.
• Payment Discounts
Consider offering an early-pay discount to insured patients with an out-of-pocket balance to provide a strong incentive to pay. Providers can use a variety discounts to lock-in payment while a patient is still at the facility – before receivables aging makes it much more expensive and difficult to collect.
Pre-pay discounts are offered during registration or follow-up financial outreach. Point-of-service and prompt-pay offers (such as a sliding-scale discount for patients in the 30 day post-encounter window) lock-in revenue up-front. All three options lessen the need for follow-up statement delivery and hands-on collection activities.
• Online Payment
Although it isn’t technically a point-of-service pay channel, online billing and payment tools are a critical part of many of the up-front collection activities discussed in this blog. That includes:
- Ensuring that pre-service estimates easily and securely accessible by patients 24/7 in an online portal.
- Self-service estimation tools – similar to those used by customer service employees – that let patients enter insurance and encounter information and receive a custom quote that can be used to compare treatment options.
- As a way for patients to manage payment plans. Online tools can help patients setup new payment arrangements, view progress on an existing plan, or make additional payments cover an outstanding balance faster.
- For transaction receipts. By linking point-of-service tools to an online payment portal, patients can track payment status or view pay history for budgeting or tax purposes.
Get Updates
Featured Articles
Categories
- Charity Care Management (1)
- Compliance (2)
- Customer Service (8)
- Digital Front Door (1)
- Direct Mail (6)
- eBilling (1)
- EBPP (34)
- ESL Statement (2)
- eStatement (1)
- Healthcare Channel Partner Billing (1)
- IVR (3)
- Mobile Payment (11)
- Online Billing and Payment (6)
- Online Patient Payment (17)
- Outsource Print Management (4)
- Paperless Billing (4)
- Patient Engagement (2)
- Patient Friendly Billing (21)
- Print and Mail (7)
- QR Codes (1)
- Quick Pay (7)
- Security (1)
- Self-Pay Patients (9)
- Self-Pay Revenue (4)
- Statement Design (32)
- Statement Print and Mail (1)
- Statement Printing and Mailing (28)
- Statement Processing (36)
- TransPromo (1)
- Up-Front Billing (1)


